Sport and exercise are important for general well-being and to help keep us healthy, but unfortunately, injuries and ill-health can also occur through sport or exercise.
Sustainable athletics
Training is based on the principle of balance between exercise load and recovery. If recovery is insufficient, then the risk of ill-health is increased. Parents of young athletes have reported that their children’s’ recovery can be negatively affected by social stress- “young people need to check their mobiles all the time” – and that sleep can be negatively affected by late training times.
Recovery can be defined as an ongoing biopsychosocial process that reduces all types of fatigue and rebuilds power and energy. If recovery needs are met then the risk of chronic fatigue, overload injury, fatigue related depression, overtraining syndrome, burnout, lack of motivation, impaired immune system function and, not least, impaired performance is reduced.
A basic rule is that the more activity the athlete is exposed to, e.g. athletics training, – the greater their need for recovery. Therefore, to ensure an athlete can take full advantage of their training, and increase their physiological performance, training always needs to be followed by sufficient recovery.
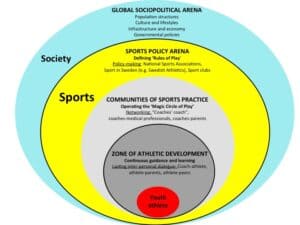
To ensure an athlete’s well-being within sport it is, therefore, important to view both the sport and the athlete from a holistic perspective. Multiple factors (at different levels) that have influence on the athlete will affect them to varying degrees. Some factors have a more direct impact on the risk of injury or ill-health, such as a lack of sleep or school related stress. Whilst other factors, perhaps more at the societal level, can also contribute, such as the general trend for all of us to move less, which in turn reduces our tolerance to loading in training (Jacobsson et al, SJMSS 2017).
Taking a holistic approach means understanding that the whole is larger than the sum of its parts and that everything must be assessed within a wider context.
Causes of injuries in youth sports
About 95 percent of the injuries in athletics are related to overload. The most common causes of overload are often associated to an imbalance between exercise load and recovery, for example;
- Exercise loads one side of the body too much or is too high intensity (i.e. it is too “hard”).
- The amount of exercise (time or intensity) is increased too quickly.
- When training moves from one surface to another, e.g. from indoors to outdoors.
- The body has not, after a previous injury, had enough time to adapt to higher training loads (i.e. training is increased too quickly).
Growth – Between approximately the ages of 12 to 15 young people are growing and most of the problems and / or injuries they experience are related to growth. For example, growth plates that have not fully developed (i.e. closed) may be sensitive to uneven stresses during such periods. Read more about this in the section on exercise and puberty.
Lack of sleep has been shown to be a risk factor for developing injuries. Young people who slept less than eight hours a night have been found to have almost double the risk of injury compared to those who slept longer. Read more about sleep.
Early specialisation to a sport (or event in athletics) may influence injury risk and some current research indicates early specialisation may be a contributing factor to increased risk of injury.
Interconnected factors – research has shown that the risk of injury increases when different factors interact, such as when exercise load and intensity increase at the same time as sleep is reduced.
But, in most sports, the strongest indicator for developing a new injury is having had a previous injury!
Injury prevention
Injuries, and the consequences of injuries, can be prevented at three levels; Primary, Secondary and Tertiary prevention.
- Primary prevention involves interventions aimed at a group of athletes who are not injured or ill. The goal here is to prevent injury from occurring at all. Primary prevention interventions might be to give advice on diet & sleep, or to provide a special injury prevention program.
- Secondary prevention involves individual athletes who have a problem. They may, for example, have suffered a hamstring strain or have heel pain caused by growing. The goal here is to ensure the athlete receives a good rehabilitation program with the aim of returning to sport as safely as possible whilst minimising the risk of reoccurrence of the injury.
- Tertiary prevention usually applies to adult athletes, but it can also apply to injured young athletes, e.g. with growth-related issues (such as Osgood-Schlatter’s disease). In this case an athlete needs management over a longer period of time – perhaps even throughout their sporting career (in the case of adult athletes). In tertiary prevention the athlete often gets a program that they need to follow for several months, or even years, with the aim of preventing the injury problems from worsening.

Injury prevention programs
To prevent injuries in athletics a holistic approach is recommended. Planning training together with recovery is very important to an athlete’s well-being. It is important that a young athlete builds an understanding of, and learns to see the connections between, what happens in the body during exercise, sleep, diet and how these factors affect performance and the risk of injury (see also # tutorials).
Within team sports, specially designed warm-up programs (primary prevention) have been shown to reduce the risk of injury if they are performed twice a week. For example, the “knee control” program designed to reduce the risk of Anterior cruciate ligament injuries.
As of today, there are no scientifically based training programs shown to prevent injuries in athletics. If you want to try a general injury prevention program in your athletics group you could try the Knee control+. To ensure the program is effective it should be performed twice a week.
Knee control+ (SWIPE)
Screening
Screening is a form of testing that a group, or individual, can perform in order to detect potential vulnerabilities in athletes before they have developed into problems. The test or examination performed should be both reliable (i.e. it measures the same thing every time the test is performed) and have high validity (i.e. it actually measures what we want to measure). What screening do we want to do in sports and why?
Movement analysis
Movement analysis aims to assess an athlete’s various movement patterns to see if any asymmetries in mobility, strength, balance etc. can be detected. Several so-called muscle / joint screening programs exist, such as The Functional Movement Screen (FMS), Kinetic Control and Bosön 9+.
However, there are currently no scientifically supported tests (screenings), for sport, that can predict who will get injured. Screening of athletes is performed primarily to discuss current and previous health status and to establish contact with the athlete. It is important to collect information about any previous injuries, how these have been rehabilitated and information regarding any current, possibly ongoing injuries or complaints. This is known as secondary and tertiary prevention.
When analysing movement of young athletes who are growing it should be kept in mind that the body grows in different phases, e.g. that the bones may have finished growing but the surrounding muscles have not grown at the same rate.
Further reading:
Why screening tests to predict injury do not work—and probably never will…: a critical review http://bjsm.bmj.com/content/50/13/776 (BJSM website)
Cardiovascular screening
Examination of healthy children is not needed, nor is examination of athletes who do not have problems.
In athletics, it is recommended that an elite athlete undergo a medical check of the heart in light of the extreme strain that elite sport entails. Bare in mind that the ECG assessment should be performed by an experienced doctor who has specialist training within sports medicine. An initial test should be done when the athlete is around 18-20 years of age, and repeated between the ages of 25 and 30.
References and further reading::
Barengo NC, Meneses-Echávez JF,Ramírez-Vélez R,et al. The Impact of the FIFA 11+ Training Program on Injury Prevention in Football Players: A Systematic Review. Int J Environ Res Public Health. 2014 Nov; 11(11): 11986–12000.
Brukner P. Brukner & Khan’s Clinical Sports Medicine: Injuries, Vol 1, 5ed, McGraw- Hill Australia. 2017.
J Jacobsson, T Timpka, J Kowalski, S Nilsson, J Ekberg, Ö Dahlström, P Renström. Injury patterns in Swedish elite athletics: annual incidence, injury types and risk factors. Br J Sports Med 2013; 47:15 941-952.
Jacobsson J, Timpka T. Classification of Prevention in sports medicine and epidemiology. Sports Med. 2015 Nov;45(11):1483-7.
J Jacobsson, D Bergin, T Timpka, et al. Injuries in youth track and field are perceived to have multiple-level causes that call for ecological (holistic-developmental) interventions: a national sporting community perceptions and experiences. Scand J Med Sci Sports. 2017 Jun 12.
Milewski MD, Skaggs DL, Bishop GA, et al. Chronic lack of sleep is associated with increased sports injuries in adolescent athletes. J Pediatr Orthop. 2014Mar;34(2):129-33.
Peterson L, Renström P. Sports Injuries. 4ed. Taylor and Francis. 2016.
Thomeé R, Swärd L, Karlsson J. Nya Motions- och idrottsskador och deras rehabilitering. SISU Idrottsböcker. 2011.
von Rosen P, Frohm A, Kottorp A, Fridén C, Heijne A. Multiple factors explain injury risk in adolescent elite athletes: Applying a biopsychosocial perspective. Scand J Med Sci Sports. 2017 Feb 16.
Certified physiotherapist. Medical coordinator Swedish Athletics. Associate Professor in Public Health/Health in Sport, with a primary research focus on health in sport.
Sverker N – Sports Medicine Physician, PhD. Chair of The Medical Committee Swedish Athletics.
Scientific publications