This section provides information on some of the most common injuries that afflict athletics athletes.
It provides special information about some injuries that can occasionally occur in the growing athletes, age groups 11-19 years, that it is beneficial to be aware of. At these ages, it is relatively unusual to have overload injuries in the shoulder or elbow regions. If a young athlete has persistent discomfort in these areas, i.e. for more than 4 to 6 weeks, a Doctor should be consulted.
Acute, traumatic injuries in athletics are relatively rare. Young athletes that sustain painful, acute (suddenly occurring) injuries should seek medical advice in order to get a diagnosis. These types of injuries are not covered on this page as they should be managed by medical professionals.
Coaches! Pay attention to, and collect information on, the injuries, illnesses and medications that the young athletes in your training group have!
Parents / Guardians! Inform the coach if your child is unwell, has pain, and if they take any medication!
Young athletes should not use pain-relieving treatments in order to train or compete!
Injuries that may occur in growing children and young people.
Hip
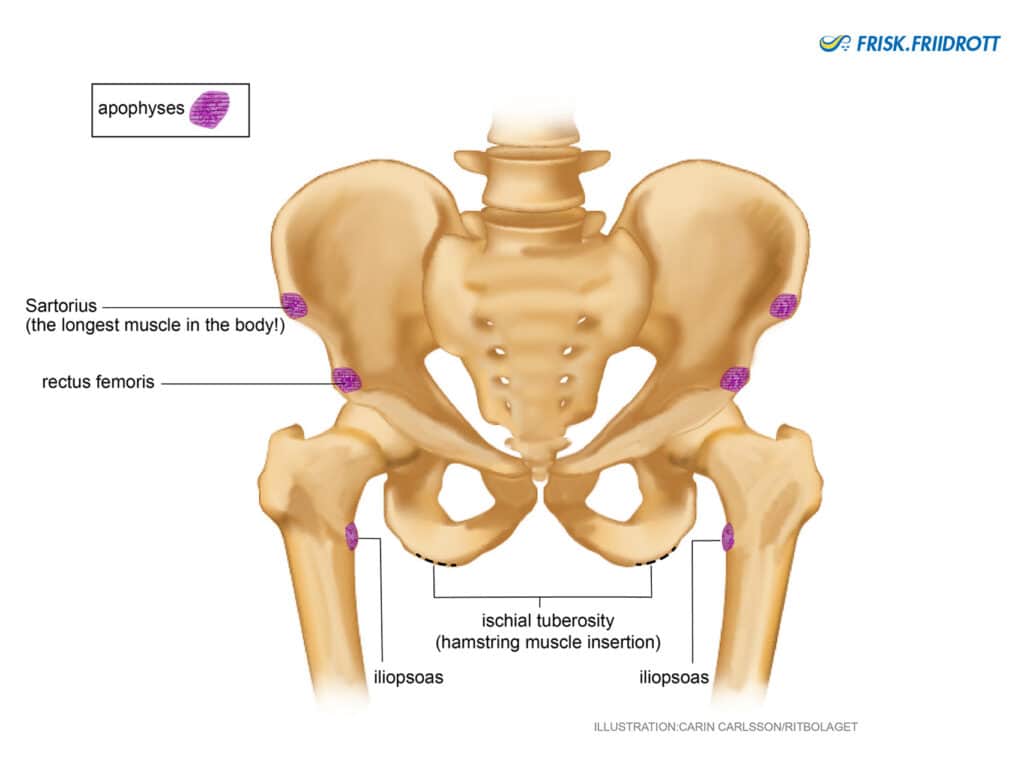
Apophyseal overload at the hip, groin and pelvis
Many muscles are attached within and around the pelvis. In growing individuals, the apophysis is the area where tendons and ligaments attach to the bone. As we grow, much of the growth takes place in the region around the apophysis. During periods in which young individuals grow fast the apophyses are more susceptible to being overloaded. Many young athletes can therefore experience problems around the hip, groin, pelvis and lumbar spine towards the end of puberty (14-18 years). N.b! In men, the apophysis around the pelvis may not be fully developed until the age of 30!
Symptoms: Gradual onset of pain at the area of muscle attachment.
Diagnosis: Clinical diagnosis (e.g. made by a doctor or other health professional without the need for diagnostic imaging such as x-rays).
Treatment: Load management (i.e. adjusting training time, type and intensity), including prompt unloading/rest at the onset of symptoms.
Rehabilitation considerations: As pain results from an overload of the apophysis and its nearby growth plate, it is important to manage training load until the pain resolves. The athlete can continue with their training, but the training load and activities should be adjusted and regularly reviewed so as not to provoke symptoms. Cross-training and activities that do not overload the painful area are recommended as substitutes for provocative training. Apophyseal symptoms usually disappear once the athlete is fully grown, but resolution can take from six months to one year. This condition is usually self-healing and benign, but if problems persist the athlete should consult a doctor.
Note! In the event of sudden onset of pain caused by an acute trauma, a so-called avulsion fracture can occur adjacent to a growth plate. This means that a small part of the bone can be pulled off where tendons or ligaments attach. Such fractures can occur, for example, at the attachment site of the hamstring or iliopsoas muscles.
Slipped upper femoral epiphysis (SUFE): ‘Slipping’ in the thigh bone growth plate
This affects growing children around the ages of 11 to 16 years old. This condition is caused by a disorder in the growth plates. It is more common in black people than white people and 2 to 5 times more common in boys than girls. The disorder rarely occurs in girls who have had their first period and occurs significantly more often in overweight children, but it can also be triggered by sports. It is possible that an endocrine (hormonal) influence may be the cause of weakening in the growth plates.
Symptoms: Pain in the groin, the front of the thigh and around the knee joint. Limping. Atrophy of the thigh muscles, i.e. muscle wasting. Reduced range of motion in the hip joint, in particular inward rotation.
It is very important that young people who notice the above-mentioned symptoms do not continue training but visit a doctor so that an x-ray can be taken!
Diagnosis: By a Doctor. Clinical examination and x-ray, plus other investigations as necessary.
Treatment: Operation.
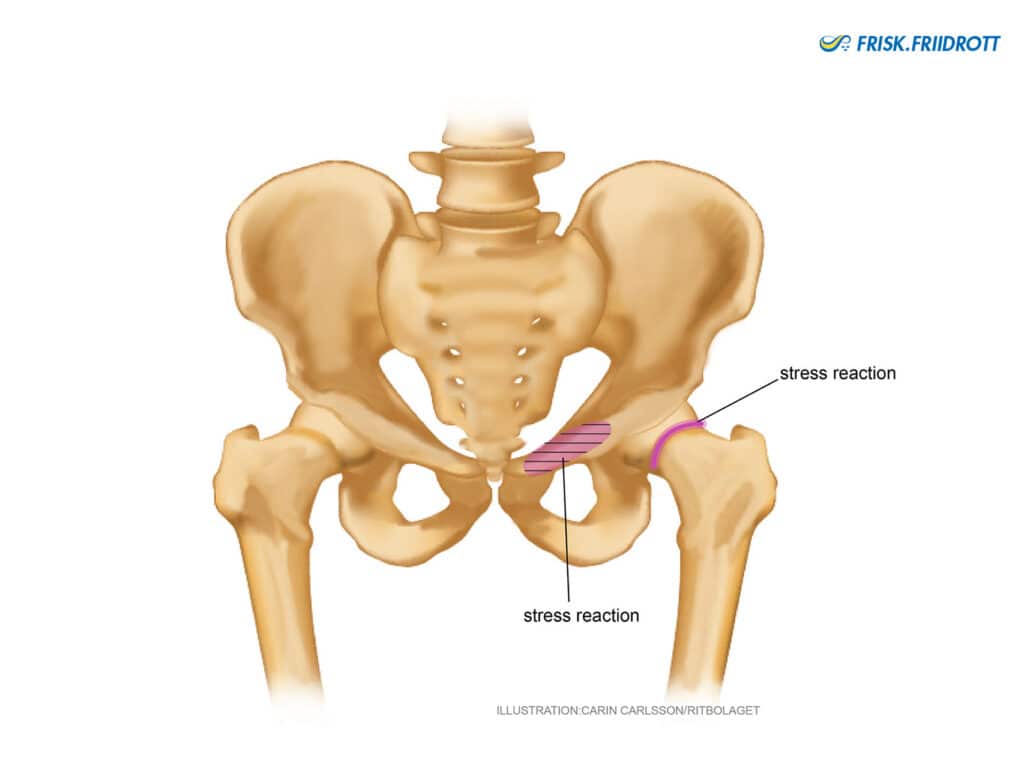
Stress fracture-stress reaction in the groin
Stress fractures occur as a result of recurrent, non-maximal, overloading. The muscles do not recover sufficiently, become exhausted and cannot dampen the loading they are exposed to. This means that the bones end up loaded instead. A small crack occurs in the outer hard (cortical) surface of the bone. This is preceded, in many cases, by an inflammation of the femur in the thigh and / or pelvic bone (so-called periostitis). Common locations of stress fractures in the groin region are the femoral neck and the area around the pubic bone (os pubis). Stress fractures can occur at any age, but are very rare in children under the age of 10.
Symptoms: Groin pain exacerbated by loading.
Diagnosis: By a Doctor.
Treatment: Protection (unloading) and rest. Possible alternative training in agreement with a doctor and / or physiotherapist.
Inflammation of the hip joint
Inflammation of the hip joint occurs often as an acute condition in children between 2 and 12 years old. This is the most common cause of hip pain (groin) in children under 10 and is more common in boys.
Symptoms: Pain in the groin and possibly the front of the thigh.
Diagnosis: By a Doctor.
Treatment: This condition usually heals itself and is benign, but it should be examined by a doctor.
Thigh
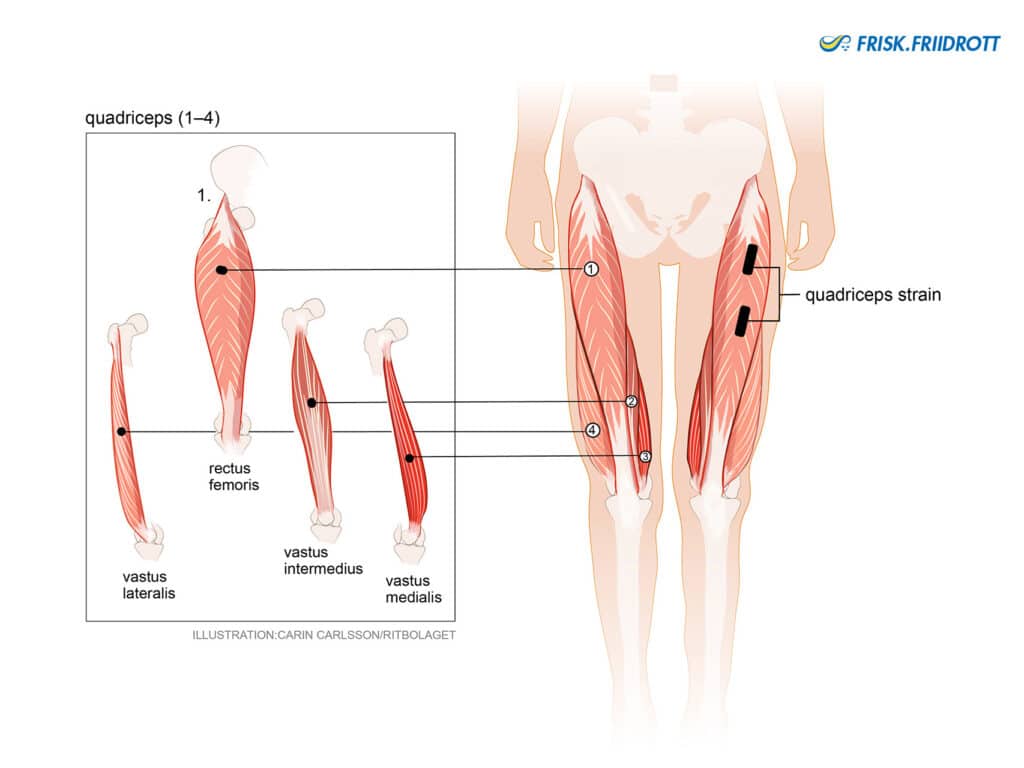
Quadriceps rupture (muscle rupture of the muscle group at the front of the thigh)
Quadriceps rupture is a relatively common overuse injury within athletics. It often occurs suddenly during sprints or jumps. Current research indicates that quadriceps muscle injury may in fact be more common than hamstring rupture amongst young athletes.
Symptoms: Sudden sharp pain in the front of the thigh (quadriceps muscles), either high up (closer to the hip) or in the lower part of the muscle (closer to the knee).
Diagnosis: Clinical diagnosis.
Treatment: Management according to PRICE (see Emergency care)!
Rehabilitation considerations: Seek advice from a physiotherapist. With good rehabilitation, this injury has a good prognosis and the athlete can usually return to athletics training after seven to nine weeks. However, if the athlete makes a premature return to sports, the risk of re-injury is high.
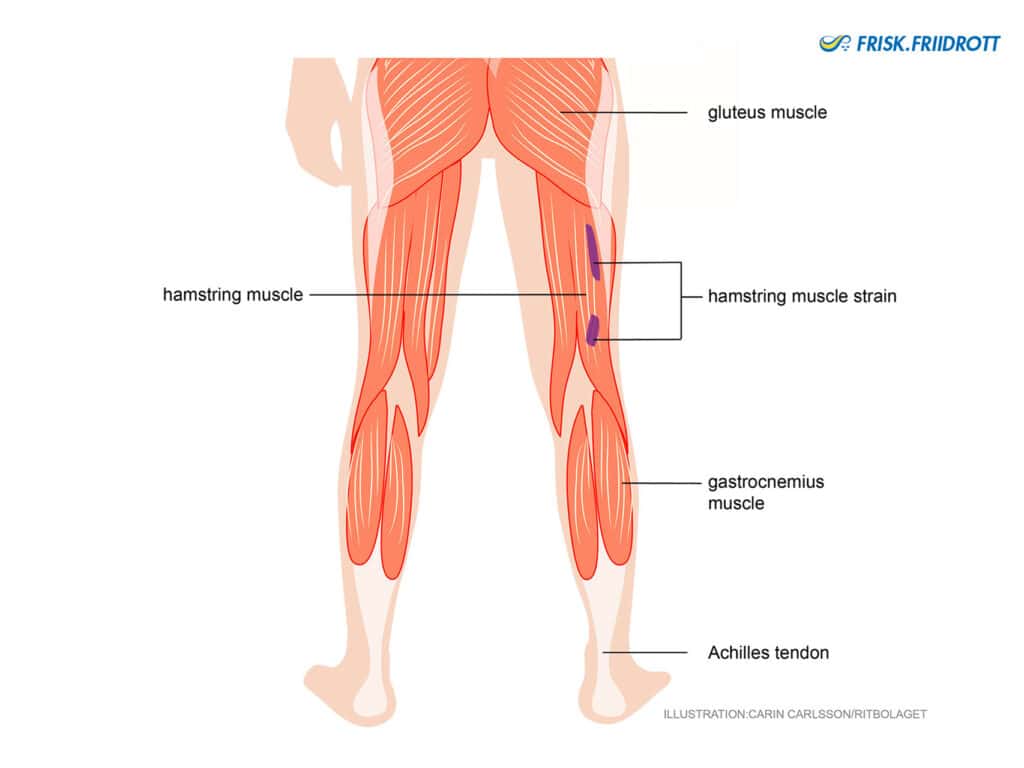
Hamstring strain
Hamstring strain (muscle pull in the back of the thigh) is a relatively common overload injury in athletics. It often occurs suddenly when an athlete sprints or jumps. Hamstring strains are not as common among young athletes.
Symptoms: Sudden stabbing pain in the back of the thigh. Can appear very dramatic.
Diagnosis: Predominantly via clinical examination (i.e. by physiotherapist or Doctor, without scans).
Treatment: It is important to employ rapid, acute care according to PRICE (see Acute Care section)! Followed by rehabilitation by a physiotherapist (the L-protocol). With effective rehabilitation, the prognosis is good and an athlete is usually back in athletics training after seven to nine weeks.
The Lengthening protocol (L-protocol)
This is a video with Carl Askling’s research-based rehabilitation program (in Swedish) for hamstring injuries, the so-called L-protocol. Research has shown that eccentric lengthening exercises are effective in rehabilitating acute hamstring injuries in sprinters, jumpers and elite football players. The program applies to both injuries of sprint and stretch type. In the event of an acute injury, it is important to have the injury thoroughly examined by a knowledgeable person before starting rehab.
The L-protocol should always be performed painlessly and can normally be started 3-5 days after the injury.
- The Extender: twice every day, 3 set x 12 reps
- The Diver: every other day, 3 set x 6 reps
- The Glider: every 3rd day, 3 set x 4 reps
Time table:
- 00.10 1. The Extender
- 01.08 Three common errors
- 02.39 2. The Diver
- 03.33 Two common errors
- 04.32 3. The Glider
- 05.13 Two common errors
Carl Askling is a certified physiotherapist, PhD. Carl works clinically in Stockholm with rehabilitation of hamstring injuries. In his research, he is affiliated with the School of Gymnastics and Sports (GIH), Stockholm.
Contact email: carl.askling@feelgood.se
Knee
Osgood-Schlatter’s disease
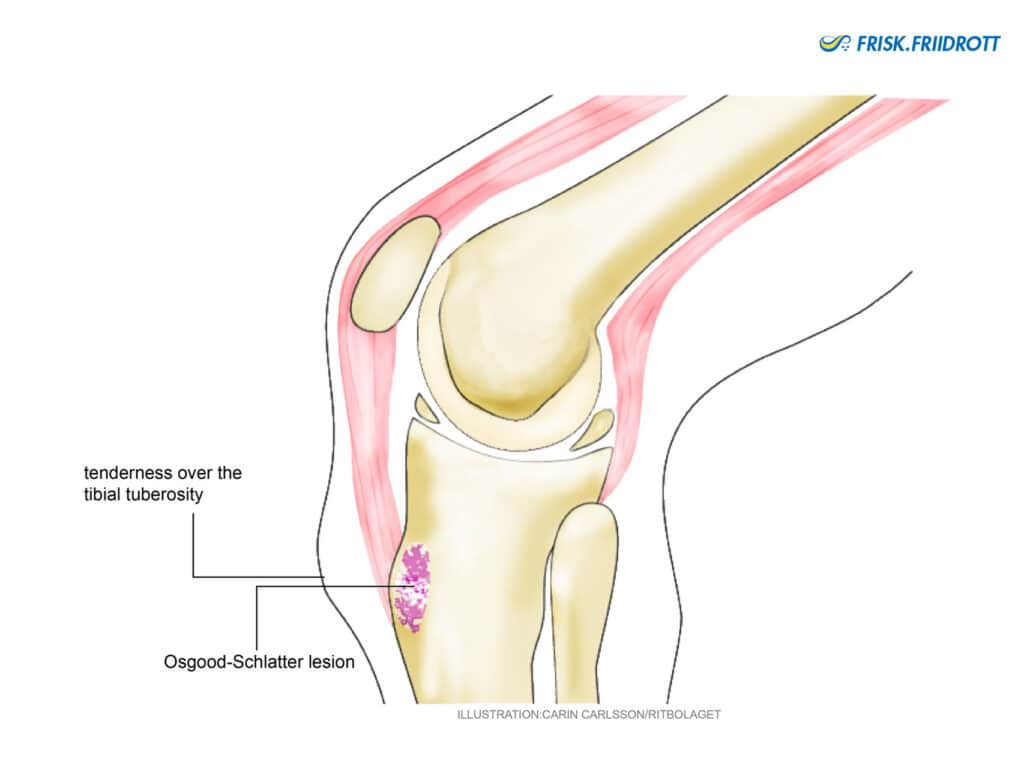
Is relatively common in young, growing athletes. It develops near the growth plate, as a result of intensive athletics. Osgood-Schlatter’s is a loosening of the tendon attachment and it is often possible to see a displacement of the tendon insertion (see picture). This usually occurs around the ages of 9 to 15, and is more common in boys, probably as they start puberty later, at an age when they begin training more intensively in sport.
Symptom: Distinctive soreness around the insertion of the patella (knee cap) tendon to the tibia (lower leg bone).
Diagnosis: Predominantly via clinical examination of a Doctor/Physiotherapist. If doubt remains an x-ray can be taken.
NOTE! These issues are related to the growing process! It is important that training is varied and adjusted!
Treatment: Avoid sporting activities that aggravate the pain. Perform alternative exercise, preferably in response the level of pain aggravation (you can use a pain scale). Unloading, protection or taping (see instruction video). The young athlete can continue to train but adaptation is important. Review the exercise plan for the coming week (current period), adjust the load on knees (jumps etc.). Refer to a physiotherapist. This condition is self-healing in most cases.
Instructional video for knee taping.(in Swedish)
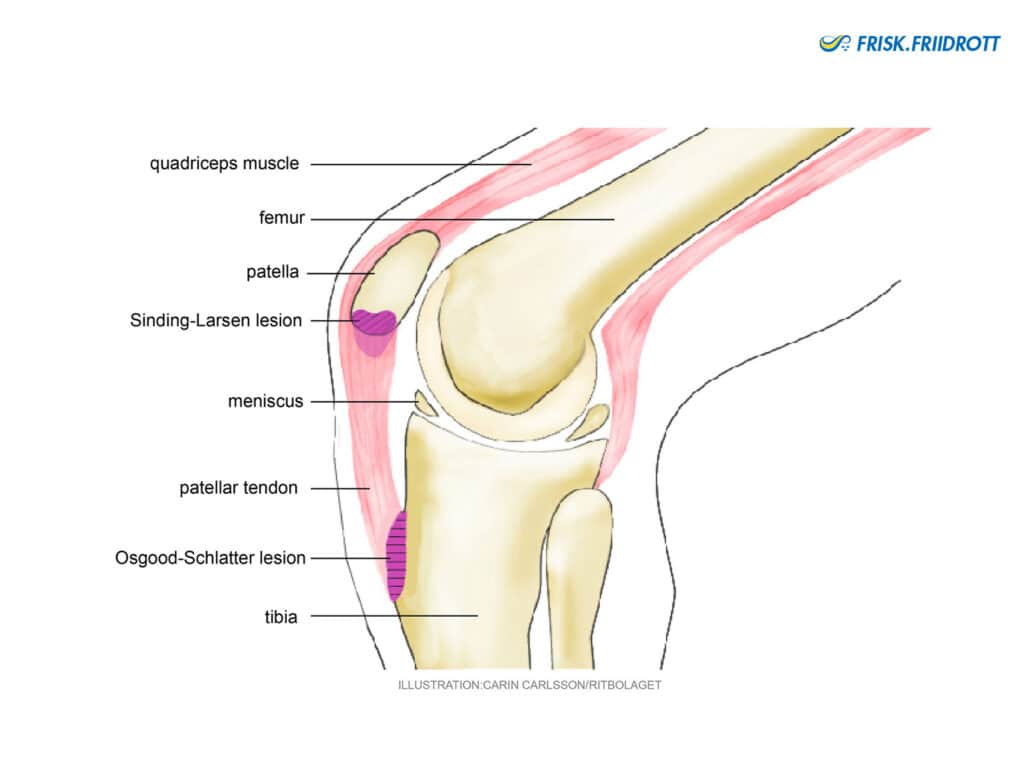
Sinding-Larsen disease
This condition resembles jumper’s knee (see below) and occurs in growing children and young people. In the growing athlete, the pain develops around the lower tip of the knee cap, and develops as a result of recurrent overloading.
Symptom: Distinctive soreness over the lower tip of the kneecap. Swelling. Stiffness. Limping.
Diagnosis: Via clinical examination by a Doctor and an x-ray.
Treatment: Symptomatic, avoid sporting activities that aggravate the pain. The young athlete can continue to train but adaptation is important. Review the exercise plan for the coming week (current period), adjust the load on the knees (jumps etc.). Early activation of the thigh muscle, see “jumper’s knee” below. This condition is self-healing in most cases and disappears when an individual is fully grown.
Osteochondritis Dissecans (OCD)-Fragmentation of bone / joint cartilage.
This is a bone and cartilage fragmentation in the knee joint that usually affects young people between the ages of 12 and 16, and is more common in boys. A crack occurs in the bone and cartilage and, in the event of fragmentation, a free body (small piece of bone/cartilage) can form in the knee joint. Usually, however, the crack heals and no fragmentation occurs. This problem is caused by small recurring traumas or overloading.
Symptoms: Pain during rest and after physical activity. Locking in the knee.
Diagnosis: By a Doctor.
Treatment: Most often self-healing, in rare cases surgery is required. Refer to a physiotherapist.
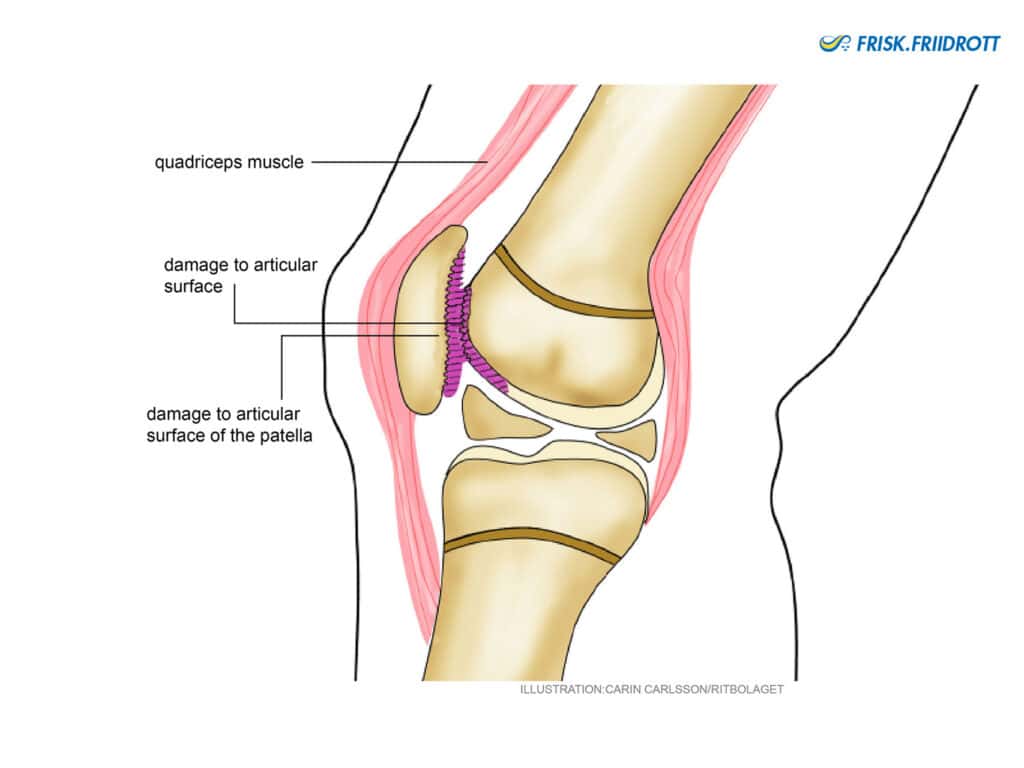
Chondromalacia Patellae/Anterior knee pain
Is an umbrella term for knee pain that occurs diffusely around the anterior (front) part of the knee joint/cap. This is more common in young girls.
Symptoms: Ache/Soreness associated to loading. Often aggravated by stairs and sitting on the heels. Usually no joint swelling.
Treatment: Avoid aggravating activity. Vary training. Strength training. Physiotherapy if required. The prognosis is good.
Jumper’s knee- Patella Tendinopathy
An overload injury in the tendon caused by intense sports. The symptoms usually develop gradually. Jumper’s knee is unusual in growing children but it can still occur (see also Osgood-Schlatter’s which is a more common cause of knee pain). Jumper’s knee is more common among boys / young men who jump frequently, this is probably as they start puberty later (compared to girls), at an age when they begin training more intensively in sport.
Symptoms: Pain around the lower tip of the knee cap (in the tendon itself). Swelling over the same area.
Diagnosis: Predominantly via clinical examination of a Doctor.
Treatment: Adaptation of loading (initial unloading). Rehabilitation with a physiotherapist. The first phase of rehabilitation is isometric (static) exercises for the anterior (front) thigh muscles (quadriceps), to achieve pain relief. Contract the muscle for about 45 sec x 5 with 2 minutes rest in between. Taping or possibly a knee support. These conditions need a longer period of rehab, of at least 3 months before adjunct measures are put in place. If symptoms do not correspond to those listed above, a Doctor should be consulted.
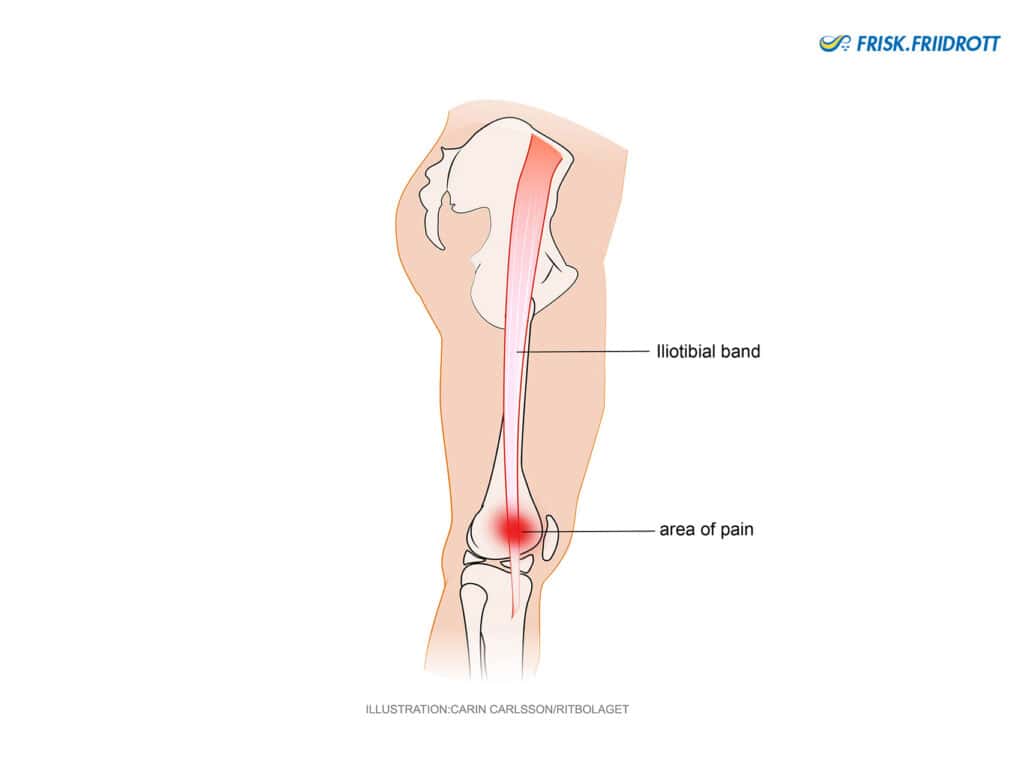
Runner’s knee (iliotibial band syndrome – ITBS)
Athletes that frequently run long distances can experience pain that is located on the outside of the knee. The cause of this pain was previously thought to be friction between the tendon (iliotibial tendon) and the underlying tissues. However, current research indicates that a “squeezing” or “compression” of local tissues is the more likely cause of runner’s knee. This ‘compression’ causes increased sensitivity in the surrounding tissues and subsequently pain.
Symptoms: Gradual onset of pain on the outside of the knee. Runner’s knee pain often occurs after about 10-15 minutes of running. This pain can increase progressively and can even become quite sharp. Downhill running can be particularly provocative. The pain often disappears after a few minutes of rest, only to reoccur when the athlete starts running again.
Diagnosis: Clinical diagnosis.
Treatment: Load management, adjustment of the athlete’s training program and cross-training. The athlete’s running style and knee function (balance, muscular control) can also be analysed and addressed when appropriate.
Rehabilitation considerations: Runner’s knee pain often occurs as a result of more monotonous running when the knees are consistently flexed at a similar angle (around 30 degrees of flexion [bend]). Therefore, it may be advisable to replace monotone runs with interval running sessions. Stretching of the gluteal muscles (including the gluteus maximus which attaches into the ITB) and the muscles on the front and outer thighs may be beneficial. Good strength around the gluteal muscles is also important. Finally, the athlete may wish to review their footwear and insoles. If problems persist the athlete should consult a physiotherapist.
Acute trauma to knee joints with joint swelling
A Doctor should always be contacted to determine if an x-ray examination is required. Treatment then follows any findings.
Young athletes who experience persistent pain in their knee or hip, i.e. pain that lasts for more than two weeks and does not improve with rest, should always be examined by a Doctor. As a pain in the thigh and knee may originate from the hip joint.
Lower leg/Heel/Foot
Sever’s disease (also called calcaneal apophysis)
Affects active, growing people between the ages of 8 and 15 years old and can, occasionally, occur in both heels at the same time. It is caused by intensive sports participation and is commonly seen in sports which require high amounts of loading of the feet and ankles, such as jumping, hopping etc.
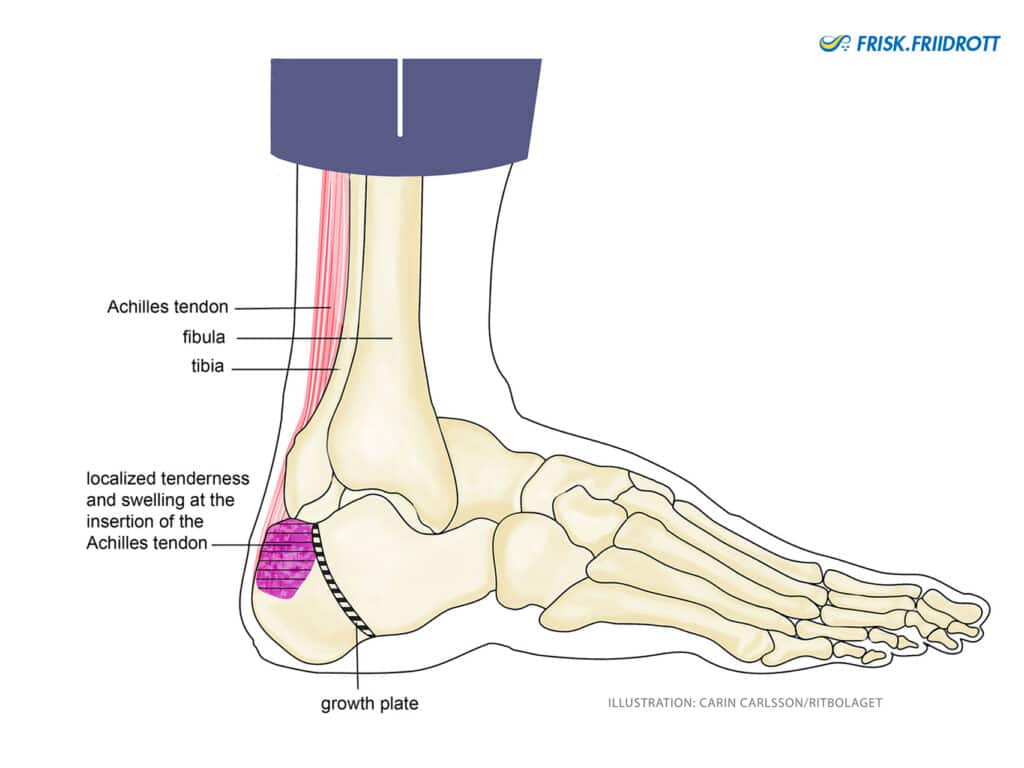
Symptoms: Pain is located on the heel bone (inside or outside), around the Achilles tendon attachment on the back of the heel. This area is often swollen and sore.
NOTE! These problems are related to the growth plates and are not overloaded tendons!
Treatment: Prompt unloading and inserts under the heel are recommended, for example using gel cushions or heel cups (see picture). During rehabilitation, it is important to remember that the pain comes from an overloaded (i.e. compressed) growth plate. This means that young people with growth plate problems should not perform similar rehabilitation programs to adult athletes that have tendon problems! It is possible to rest and unload until the pain is gone. You can continue with varied exercise and activities that do not load the feet and heels. A young athlete can continue to train but adaptation is important, review the plan for the coming week, and adjust the amount of loading on the feet/heels (jumps etc.). The prognosis here is always positive. The discomfort usually disappears when the individual is fully grown, but it can take up to six months, or a year, before the problem has fully healed. In case of long-term problems, medical advice is recommended.
Haglund’s deformity – is a bony enlargement on the back of the heel.
Instructional video for taping of the heel. (in Swedish)
Mid portion Achilles pain
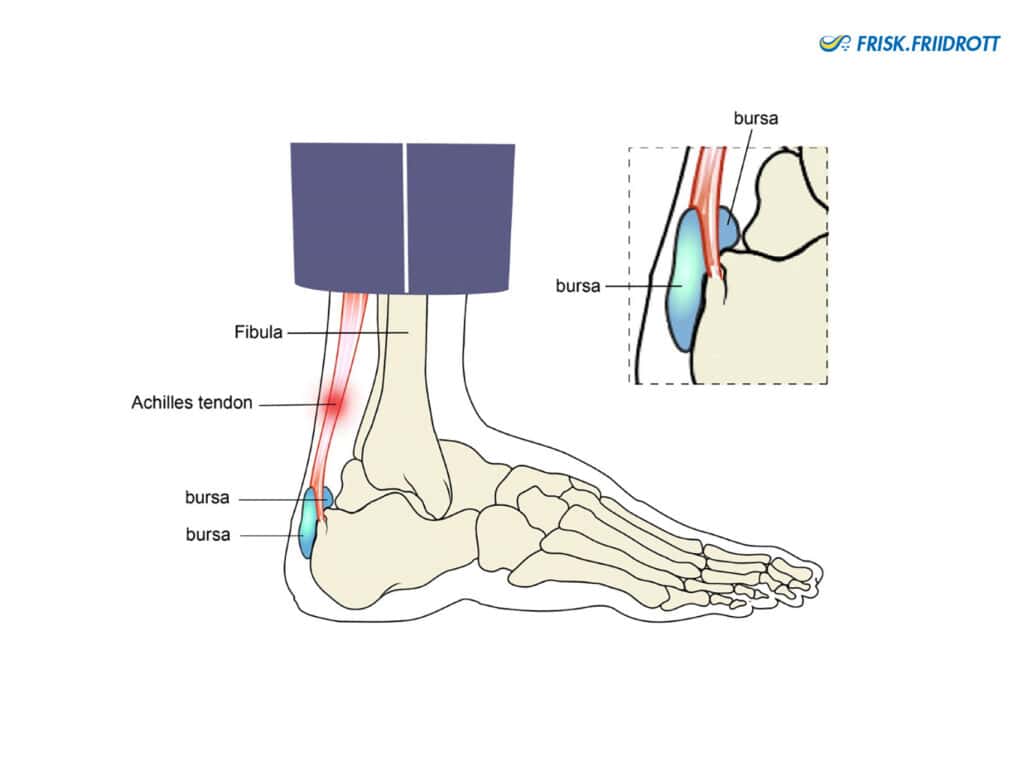
Achilles pain is a relatively common overuse injury seen in athletics. Achilles problems are generally divided into two. First, where the pain is located in the main body of the tendon (2-6 cm up from the heel bone) and second, where the pain is located at the site the tendon attaches onto the heel bone. In the latter, it is often a bursa (fluid filled membrane) that becomes irritated and painful (NB. In the growing athlete, it is often the growth plate or apophysis that becomes irritated and this requires different management; see the page on Severs).
Symptoms: Tendon pain and stiffness in the morning. The tendon is often tender when pressurised and may be swollen. Achilles pain can often improve during activity or warming up before worsening again.
Diagnosis: Clinical diagnosis, with or without ultrasound.
Treatment: In both types of Achilles tendon pain, an irritated bursa (pain near the heel bone) and irritated mid-portion of the tendon (2-6cm above the heel bone), it is important to initially protect the tendon from provocative activities. An athlete with pain at the heel bone should also review their footwear to check if their shoes are pressing onto the heel.
Rehabilitation considerations: Loading/strengthening and load management. Research shows that all types of calf strength training (eccentric, isotonic, isometric) can be used to improve the load tolerance of the tendon. The program should be individually tailored and the increase in load should be progressive. These conditions need a longer period of rehab, of at least 3 months before adjunct measures are put in place.
Example of a rehabilitation program for heel pain:
Phase 1. Pain management: Continue with activities that cause pain at a level of 0-3 on a 0-10 scale (0 = no pain), for example, aqua-running or cycling.
Phase 2. Recovery and rebuilding: Increase the strength of the calf muscles and the strength of the tendon. E.g. begin with bilateral (both feet) heel raises from the floor daily. When the pain subsides, start heel raises on one leg, preferably slowly, from the floor, e.g. 3×6 times, 3 times a week.
Phase 3. Gradual increase in loading: One-legged heel raises with additional heavy load, e.g. in a Smith machine 2-3 times / week, approx. 3×8-10 reps. Remember to press all the way up with the big toe! Add in running activities and jumps. Continue to monitor the pain levels in order to guide progress.
Phase 4. Return to normal training.
Tennis leg
‘Tennis leg’ is a muscle injury / rupture in the middle of the calf which occurs more commonly in older athletes. The injury occurs in the connective tissues between the two primary calf muscles (Soleus and Gastrocnemius). The injury is usually acute (sudden) but the underlying cause is often overuse.
Symptoms: Acute pain in the middle of the calf. It is important not to confuse this injury with rupture of the hamstring.
Diagnosis: Clinical diagnosis plus ultrasound.
Treatment: In the acute phase, treatment follows PRICE recommendations and includes use of pressure bandages. Rehabilitation follows and usually takes around 4 to 6 weeks. Symptoms subside relatively quickly but healing often takes up to 2-3 months. Therefore, if the athlete makes a premature return to sports, the risk of re-injury is high.
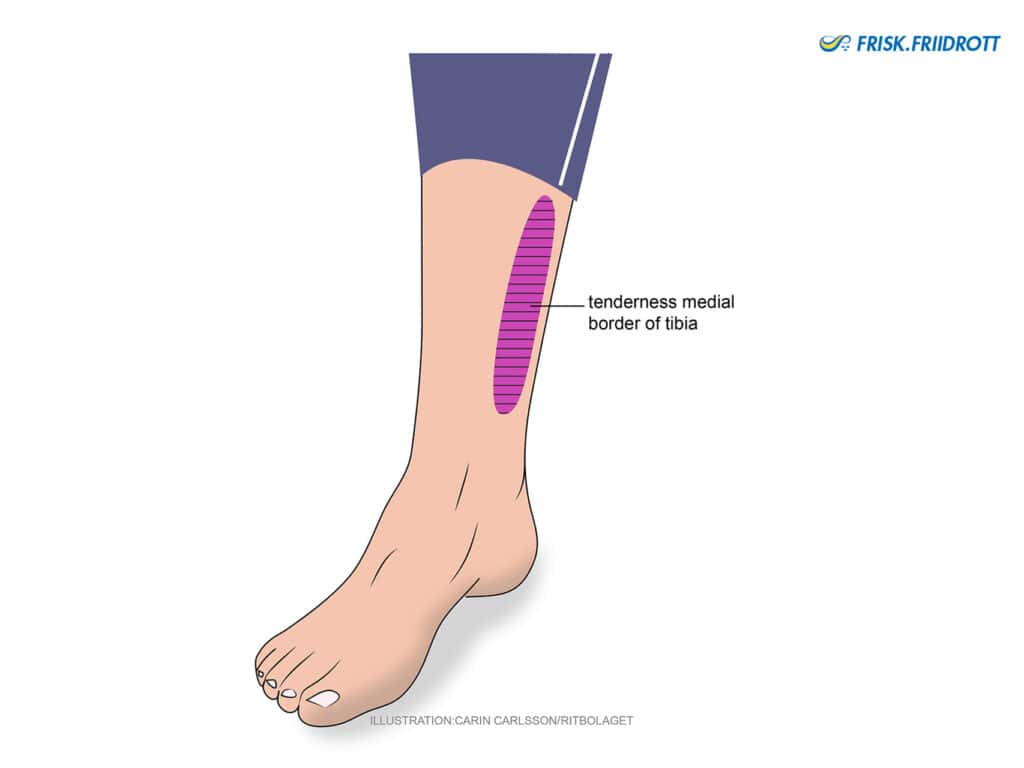
Medial tibial stress syndrome (MTSS)- Shin splints.
Is common in young athletes. The cause is often overloading and this usually occurs when changing surfaces or training type, for example when you start training indoors in the autumn or start training with more hopping.
This can be prevented by ensuring a more gradual transition between types of training sessions and environments, for example, by delaying the use of spikes. Try to review the balance between exercise load and recovery and check you have well-fitting shoes.
Symptoms: Tenderness/soreness along the inner edge of the tibia (shin bone). Some swelling can occur over the same area. The symptoms are often exacerbated by continued loading.
Diagnosis: Predominantly via clinical examination.
Treatment: Stop training following the onset of symptoms, and exercise in ways other than running and hopping. Rest followed by guided exercise. Physiotherapy as necessary. The return to athletics should be gradual, for example, by starting with warm-up jogging and coordination intervals and delaying the reintroduction of jumping. Should symptoms persist other treatment may be required. Seek medical attention if the symptoms do not resolve after 4 to 6 weeks, or if the pain is very localised, i.e. the size of a one-pound coin.
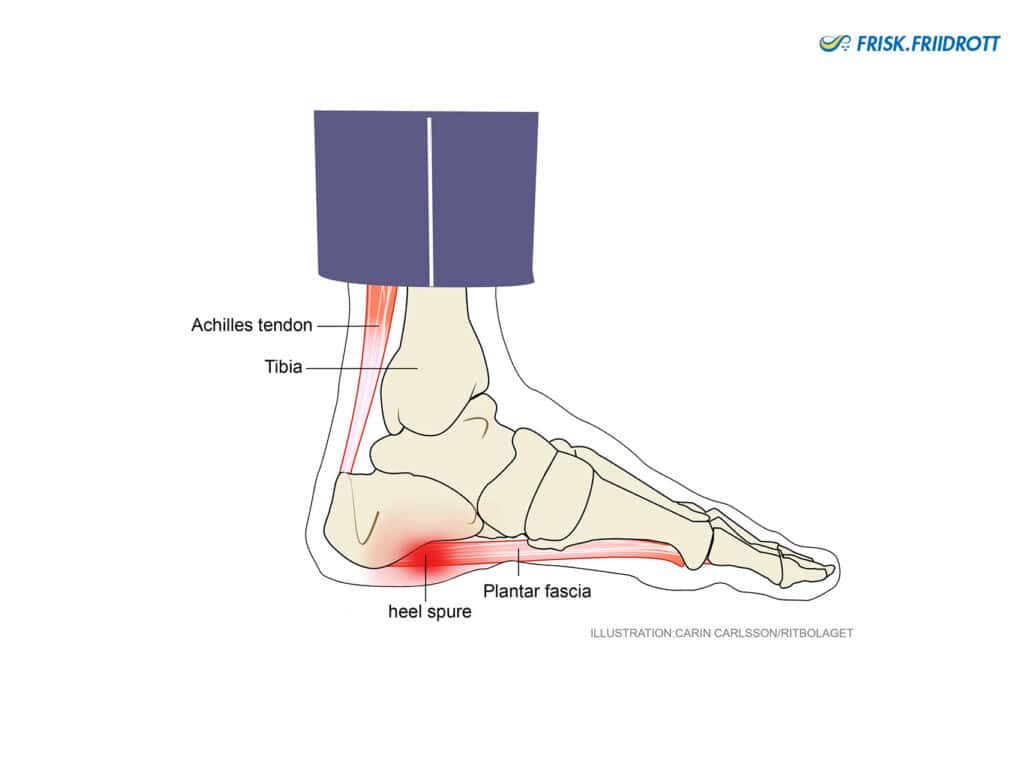
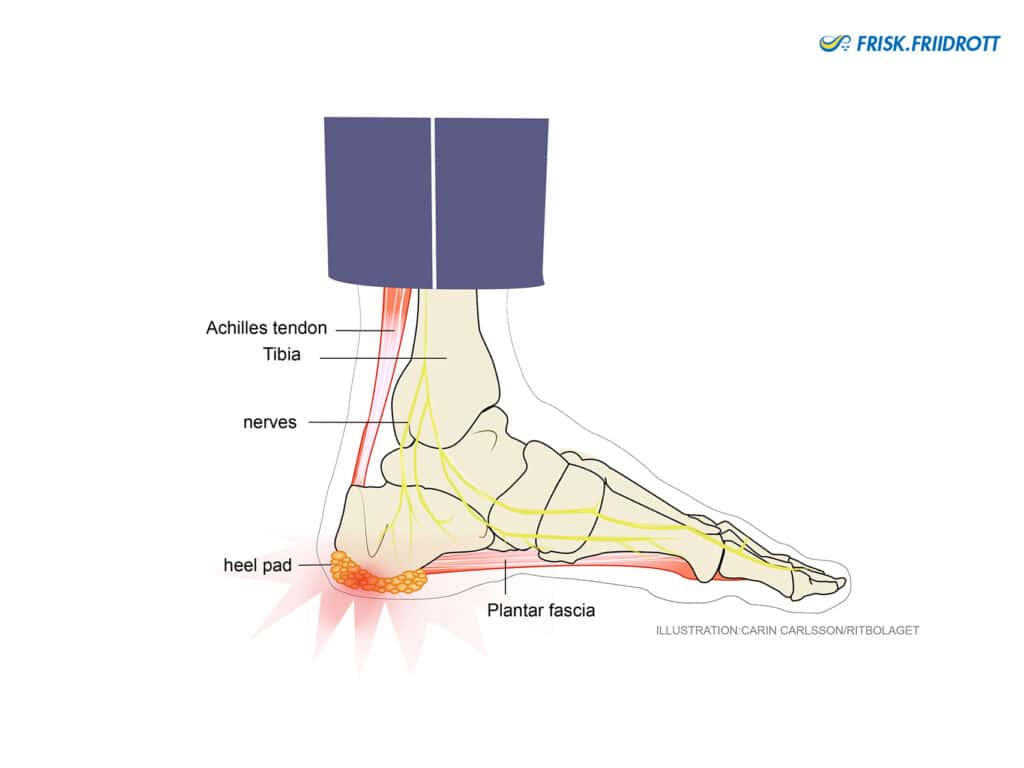
Heel spur (plantar fascia pain)
The plantar fascia is a large flat tendon located under the foot. In some athletes repeated overloading, for example through running and jumping, can cause small ruptures in the tendon where the tendon attaches to the heel bone. If the initial pain is ignored and the overloading continues persistent pain can develop. In older athletes, the plantar fascia is more fragile and healing can take a long time. For differential diagnosis, see the section on nerve impingement below.
Symptoms: Pain under and/or on the inside of the heel during exercise.
Diagnosis: Clinical diagnosis.
Treatment: Initial unloading/rest. The athlete should review their footwear (in particular the cushioning in their shoes), the surfaces on which they train as well as their total training load.
Rehabilitation considerations: Some training activities can be more provocative for the plantar fascia than others, in particular jumping, high-speed and long-distance running. A forefoot running style may also stress the fascia more.
Rehabilitation should include strength training of the forefoot and the muscles around the ankle. During strength training of the calf muscles it is of particular importance to focus on pushing all the way up through the big toe. Taping to assist shock absorption can also be used. A rehabilitation program for plantar fascia pain can follow the same principles as the Achilles tendon, see above. Recovery from plantar fascia pain can take a long time, from months to even years, so early action is important.
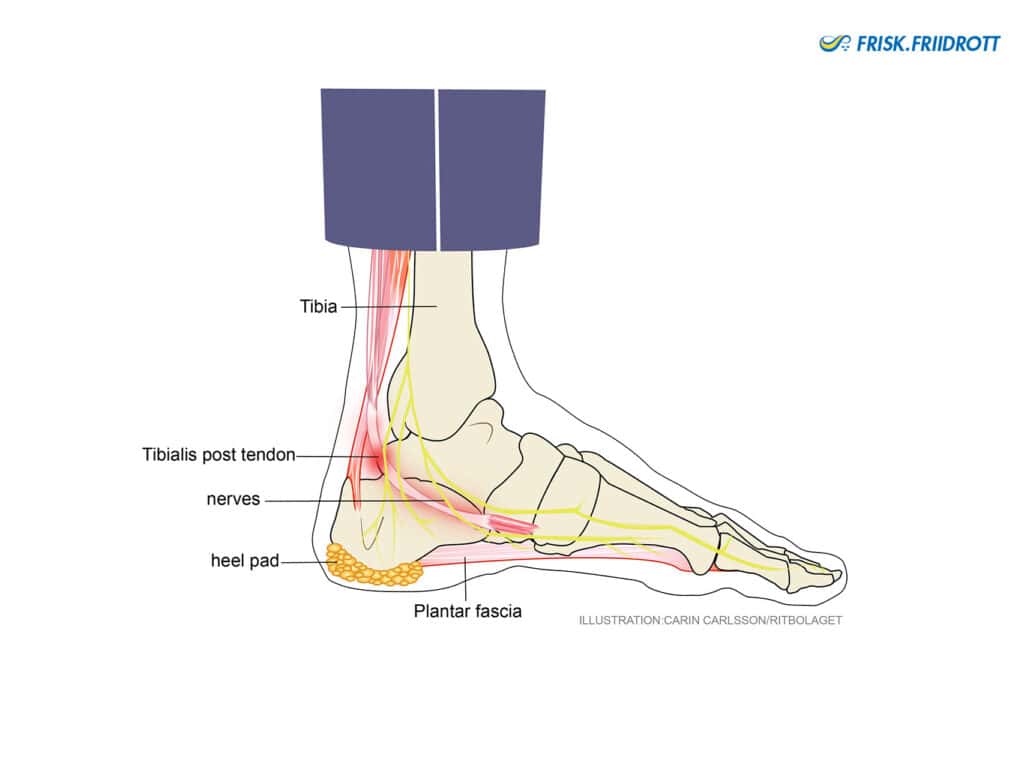
Nerve impingement or tendon dysfunction
There are several structures around the heel and ankle that can become sensitive and painful.
Symptoms: If the nerve that is located close to the heel bone (so-called calcaneus nerve or “Baxter’s nerve”) becomes irritated symptoms similar to plantar facia pain can occur. Pain located on the inside of the ankle, behind or below the ankle bone and slightly higher up than the heel, may be attributed to an overloaded local tendon (m. Tibialis posterior). The tibialis posterior muscle functions to help stabilise the medial longitudinal arch of the foot. Weakness of the tibialis posterior muscle can contribute to flat feet.
Diagnosis: Clinical diagnosis.
Treatment: Initial unloading/rest.
Rehabilitation considerations: Strengthening of the muscles of the forefoot and the muscles around the ankle. The program should be individually tailored following diagnosis.
Heel pad syndrome
Heel pads are located under the heel bone. These heel pads are primarily made up of fatty tissue and have a shock-absorbing function. However, with repeated loading, such as jumping, the heel pad can flatten out and its ability to absorb shock can deteriorate.
Symptoms: Gradual or acute onset. Pain under the heel which is aggravated by loading. The pain is often worse during barefoot walking.
Diagnosis: Clinical diagnosis.
Treatment: Initial unloading/rest. Review footwear and insoles. Consider taping, heel-cups or orthoses. Heel pad syndrome usually resolves but it may take time.
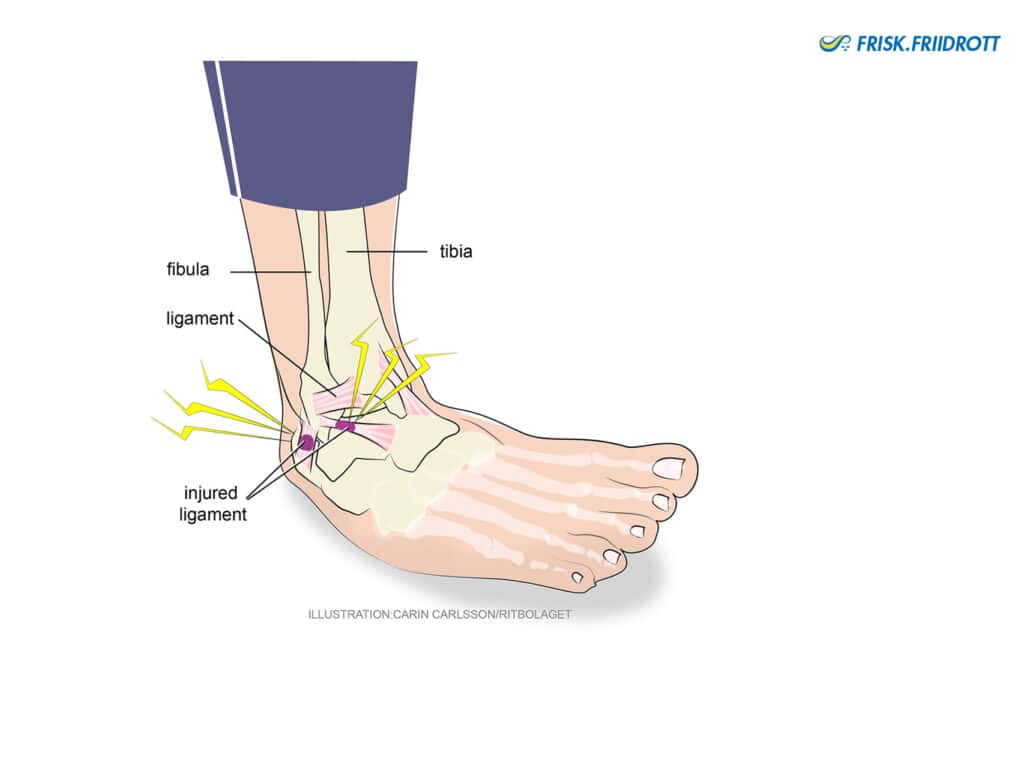
Ankle sprain
Twisting an ankle, i.e. turning the foot inwards, is, unfortunately, common in sports. Most commonly this leads to injury of the ligaments on the outside of the ankle and bleeding occurs if a ligament is ruptured.
Symptoms: Acute/sudden onset. The athlete twists the ankle, with the foot turning inwards and often under the body.
Diagnosis: Predominantly via clinical examination. If an athlete cannot weight-bear on the foot after 4 to 7 days then a Doctor should be consulted for further investigation.
Treatment: It is important to take action quickly, via acute care with PRICE/POLICE! Rehabilitation with a physiotherapist. The prognosis is good. In the case of less severe ankle sprains, balance training can start early (i.e. after 2-3 days), this can begin first on the floor, on a soft surface. During the first weeks after an ankle sprain, the injury is vulnerable and there is an increased risk of exacerbation (by twisting the ankle again). As such it is important to continue balance exercises for 4-8 weeks after the injury, preferably supplemented with ankle strengthening exercises.
Shoulder
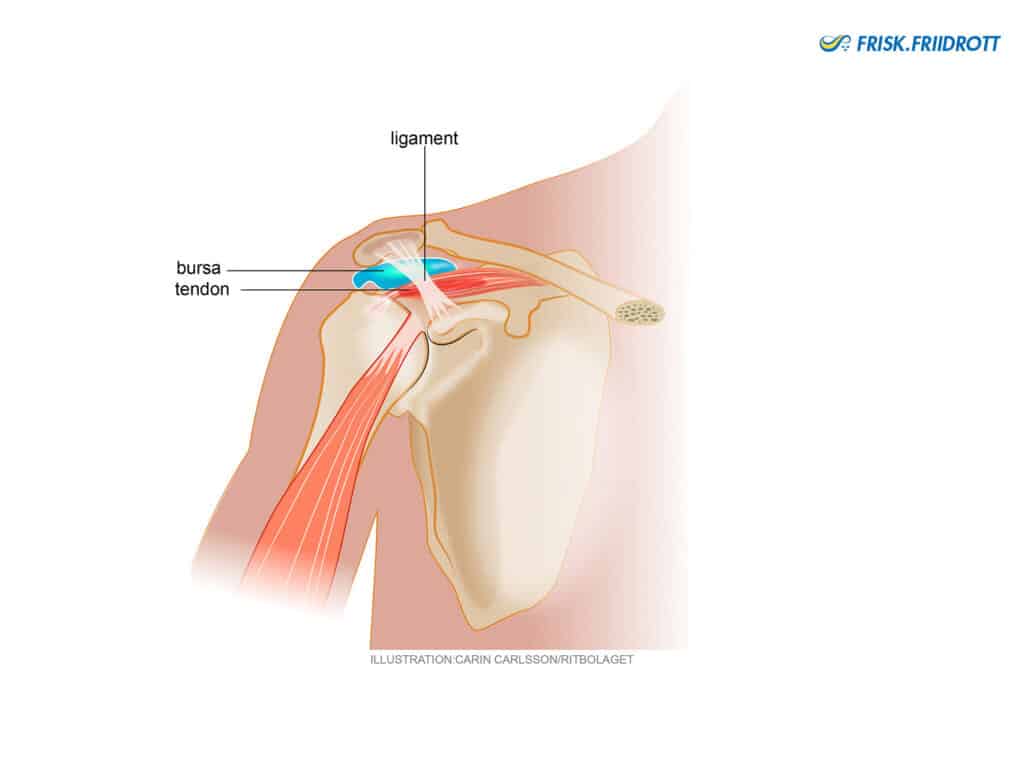
Shoulder impingement
Shoulder impingement syndrome is not a specific diagnosis, but more of an umbrella term for a multi-factorial syndrome. Traditionally it has been supposed that a structure within the shoulder (e.g. a tendon or bursa) has become “squeezed”. Impingement syndrome is usually divided into primary and secondary impingement. Primary impingement is classified as a condition where the anatomical space in the shoulder is thought to be “too small”. This form of impingement usually inflicts older athletes. Younger athletes, around the age of 20, usually have so-called secondary impingement. Secondary impingement is thought to be caused by a combination of a too large shoulder joint capsule and inadequate function of the shoulder muscles. These factors lead to inadequate dynamic control of the shoulder ‘ball’ in its ‘socket’ which causes irritation of local structures.
Symptoms: Pain when moving and loading the shoulder. Primarily when the arm is above shoulder height. Symptoms of primary and secondary impingement are similar.
Diagnosis: Primarily clinical diagnosis. Ultrasound or MRI scans may be indicated in certain cases. Consultation with a doctor and/or physiotherapist is often recommended, as it can be important for athletes with impingement type problems to understand which factors are contributing to their symptoms.
Treatment: Initial unloading/rest. Rehabilitation should incorporate training that targets the local shoulder muscles and shoulder blade stability. Taping can be considered. Contact with a physiotherapist is recommended to ensure the rehabilitation program is individually tailored to the athlete’s age and event.
Rotator cuff tear (shoulder stabilisers)
The shoulder joint is very mobile and as a result it relies heavily on the surrounding muscles (in particular the rotator cuff) to centre the shoulder ‘ball’ in the ‘socket’ during movements. In the young athlete, injuries/overloading to the rotator cuff usually occur as a result of repeated throwing above shoulder height, where the final phase of the throw stretches the surrounding muscles and ligaments. This can lead to an ‘imbalance’’ in the joint. It is uncommon for rotator cuff problems to be caused by ‘impingement’ in younger athletes. In older athletes however, tendons can be more fragile and an ‘impingement’ syndrome in the shoulder may lead to weakening of the tendons and their attachments (read about impingement above).
Symptoms: Pain on the front and/or top of shoulder and even on the side of the upper arm. The pain is provoked by movements above shoulder height. In the event of a more severe tendon rupture, it may be difficult to lift the arm.
Diagnosis: Primarily clinical diagnosis. Ultrasound or MRI scans may be indicated in certain cases. Consultation with a doctor and a physiotherapist is recommended.
Treatment: Initial unloading/rest. Rehabilitation should incorporate training that targets the local shoulder muscles and shoulder blade stability. Taping can be considered. Contact with a physiotherapist is recommended to ensure the rehabilitation program is individually tailored to the athlete’s age and event.
Elbow/hand
In throwing sports the elbow and hand can be exposed to heavy loads. Some conditions associated with overloading of the elbow and hand are:
- Rupture / partial rupture of ligaments on the inside of the elbow (medial collateral ligament) (common in javelin).
- Overuse of the muscle attachments on the outside or inside of the elbow (lateral and medial epicondylitis [tennis and golfers elbow]) (common to all throws).
- Pain located at the back of the elbow can be due to so-called free bodies within the joint (common in shot-put and javelin).
- Partial muscle strain of the finger and/or wrist flexors resulting in pain at the medial (inner) condyle of the elbow (javelin)
Diagnosis: Primarily clinical diagnosis. X-rays or MRI scans may be indicated in certain cases
Treatment: Initial unloading/rest with onset of pain. Prompt contact with a physiotherapist, hand therapist, or doctor is strongly recommended!
Back
Back problems in children under 10 to 12 years old are very rare. Back pain is much more common when children reach puberty and go through periods of rapid growth. Young athletes around 16-19 years of age, who also train at the elite level, more often suffer back pain compared to young athletes of a similar age who exercise at a lower level.
Symptoms: Pain in the lower back (lumbar spine) associated with loading.
Diagnosis: Predominantly via clinical examination. In many cases, the back pain of these elite athletes has a so-called structural explanation that cannot be detected with regular clinical examination, therefore, supplementary investigation, for example, with an MRI scan may be needed.
NOTE! Back problems around these ages (16-19) are often related to the final stages of growth!
Treatment: Stop training following the onset of symptoms, and exercise in ways other than running and hopping. Rest followed by guided exercise. Referral to a physiotherapist. Return to athletics should be gradual. You can also read the sections on Exercise and Puberty, and Growth.
In the case of persistent complaints, it should be noted that there are causes of back pain in children that require consultation with a Doctor, to seek a diagnosis and prompt treatment (e.g. stress reactions / fractures, tumors, herniated discs, spondylitis, congenital kyphosis, etc.).
Read more research about back pain; Back problems common to elite athletes.
Stress fractures
Stress fractures can occur in a healthy bone if repeated overloading is not balanced with sufficient recovery. The affected bone first swells, known as a stress reaction (bone marrow oedema), then, if overloading continues, minor cracks may begin to appear in the bone tissue. Common sites for stress fractures in athletes involved in athletics are the vertebrae in the lumbar spine (L5), the sacrum, the femur (thigh bone), the inside or front of the lower leg (tibia), and the navicular bone of the foot.
Symptoms: Symptoms often initially present as a localised pain that increases during exercise and disappears during rest. The pain is a warning signal and it is therefore important to ‘listen to the body’ and stop provocative activity! If the imbalance between loading and recovery is not addressed, the pain increases and weight bearing activities eventually become impossible. Extra attention should be paid to pain in the lower back (lumbar spine) and sacrum as these stress reactions / fractures can be mistaken for benign back pain.
Diagnosis: Through MRI after consultation with a doctor.
Treatment: Initial unloading/rest with onset of pain. Some stress fractures can take a very long time to heal. For example, stress fractures in the back, lower leg and navicular bone in the foot can take up to 6 to 10 months to heal.
Rehabilitation considerations: A fracture heals at its own pace and it is not possible to speed up the healing process. As such, it is important to protect the bone from overloading and give it sufficient time to heal. It is also necessary to ensure sufficient energy (calories) and nutritional intake during the healing process. Training such as aqua-running and general conditioning can be used as a substitute for normal training activities. Rehabilitation should be guided by a physiotherapist and the return to athletics should be made gradually. Finally, it is important to review the factors that may have contributed to the development of the stress fracture and ensure a better balance between loading and recovery on return to athletics.
Frequently asked questions:
What are the most common symptoms of an overload injury?
An overload injury usually builds up gradually, for example, by beginning with a feeling/awareness in the foot or lower leg that something doesn’t feel quite right. Often this feeling/awareness is fairly well-localised to an area or point.
When can an athlete return to competing after an injury?
In order to reduce the risk of reoccurrence of injury (or a new injury), an athlete should have been able to exercise normally for two weeks prior to any competition.
Written by: Lena Haggren Råsberg and Jenny Jacobsson
Instructional video: Tommy Eriksson
References and tips for further reading:
Askling CM, Tengvar M, Thorstensson A. Acute hamstring injuries in Swedish elite football: a prospective randomised controlled clinical trial comparing two rehabilitation protocols. Br J Sports Med. 2013;47(15):953-959. doi:10.1136/bjsports-2013-092165
Askling CM, Tengvar M, Tarassova O, Thorstensson A. Acute hamstring injuries in Swedish elite sprinters and jumpers: a prospective randomised controlled clinical trial comparing two rehabilitation protocols. Br J Sports Med. 2014;48(7):532-539. doi:10.1136/bjsports-2013-093214
Brukner P. Brukner & Khan’s Clinical Sports Medicine: Injuries, Vol 1, 5ed, McGraw- Hill Australia. 2017.
Challoumas, D., Crosbie, G., O’Neill, S. et al. Effectiveness of Exercise Treatments with or without Adjuncts for Common Lower Limb Tendinopathies: A Living Systematic Review and Network Meta-analysis. Sports Med – Open 9, 71 (2023).
Danielsson och Willners Barnortopedi. Studentlitteratur. 2006.
Peterson L, Renström P. Sports Injuries. 4ed. Taylor and Francis. 2016.
Smith MD, Vicenzino B, Bahr R, Bandholm T, Cooke R, Mendonça LM, Fourchet F, Glasgow P, Gribble PA, Herrington L, Hiller CE, Lee SY, Macaluso A, Meeusen R, Owoeye OBA, Reid D, Tassignon B, Terada M, Thorborg K, Verhagen E, Verschueren J, Wang D, Whiteley R, Wikstrom EA, Delahunt E. Return to sport decisions after an acute lateral ankle sprain injury: introducing the PAASS framework-an international multidisciplinary consensus. Br J Sports Med. 2021 Jun 22:bjsports-2021-104087. doi: 10.1136/bjsports-2021-104087.
Silbernagel KG, Hanlon S, Sprague A. Current Clinical Concepts: Conservative Management of Achilles Tendinopathy. J Athl Train. 2020 May;55(5):438-447. doi: 10.4085/1062-6050-356-19. Epub 2020 Apr 8. PMID: 32267723; PMCID: PMC7249277.
Sundell CG. Low back pain in adolescent athletes. Umeå University medical dissertations, 2019.
Thomeé R, Swärd L, Karlsson J. Nya Motions- och idrottsskador och deras rehabilitering. SISU Idrottsböcker. 2011.
Sports Medicine Physician, pediatric orthopedics, chief physician Astrid Lindgren’s Hospital, Stockholm. Head physician Swedish Athletics.
Certified physiotherapist. Medical coordinator Swedish Athletics. Associate Professor in Public Health/Health in Sport, with a primary research focus on health in sport.